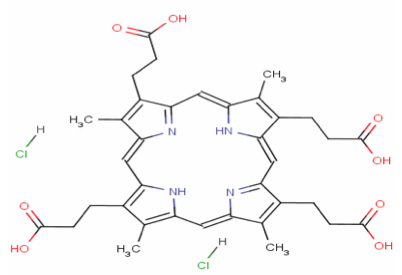
Shedding New Light on Acne: The Effects of Photodynamic Therapy on Propionibacterium acnesAcne TreatmentThe belief that upon infection one has to let acne run its course is a myth. This is because without treatment, dark spots and permanent scars can appear on the skin even after acne clears (American Academy of Dermatology, 2012). Thus far, acne treatments have targeted P. acnes with antibiotics, as P. acnes has been shown to be susceptible to a wide range of antimicrobial molecules. Families of antibiotics including quinolones, cephalosporins, pleuromutilins and sulfonamides are active against P. acnes (Torpy, 2004). However, recurrent treatment has resulted in the emergence of antibiotic resistant P. acnes, rendering treatment of acne with antibiotics ineffective. In addition, treatment with facial creams, such as Neutrogena and Clean and clear had proven effect against acne, but the benzoyl peroxide contained in these creams cause severe damage to other parts of healthy skin (Jemec, 2004). As a result of, supplementary means of treatment against excessive P. acnes have been deemed necessary. Currently, light-therapy is used as an alternative means of treatment for acne vulgaris. Light, as a form of treatment, has a long history in both oriental and western medicine (Elman, 2004). But it is only recently, as lasers and other light-based devises have become more accessible, that light has been used to treat skin-related ailments such as acne. Although the beneficial effects of light-therapy have been known by dermatologists for over thirty years, the specific wavelengths responsible for the effects were unspecified. Nonetheless, recent advancement in photomedicine has paved the way for better understanding of the processes of light therapy and accurate identification of the wavelengths of light responsible for favorable effects. Research over the past decade has offered an alternative form of acne treatment in photodynamic therapy. Photodynamic therapy (PDT) is a relatively new form of light therapy that utilizes laser technology. It is still undergoing extensive research but some aspects of the treatments are known. PDT uses light of a specific wavelength to excite a photosensitizer—a compound capable of absorbing photons (particles of light) and initiating a photochemical reaction (Elman 2004). PDT depends on three essential components—the excitable compound (the photosensitizer), light and oxygen molecules (Elman 2004). When light of a specific wavelength is shined upon a cell containing a photosensitizer, the compound absorbs the light and becomes excited. If the photosensitizer is near an oxygen molecule, the energy it absorbs is transferred to the oxygen, whereupon it creates an excited singlet state oxygen molecule (Midgley, 1984). Singlet oxygen is a highly reactive molecule that is extremely unstable and capable of dangerously reacting with and damaging surrounding cells. It is destructive and usually does not have any positive health effects. And common antioxidants, such as Vitamin C, are essential in preventing such damages by singlet oxygen and other highly reactive molecules in various parts of the body. However, in this case, singlet oxygen is beneficial because it aids in the destruction of the unwanted and excessive P. acnes bacterial cells in the skin. As follows, singlet oxygen reacts with biomolecules that are in close proximity to itself, generating a toxic environment to the surrounding cells. Following the reactions, the damaged cells are destroyed by means of apoptosis—programmed cell death—or necrosis—premature cell death (Delany, 1991).Figure 2. Corproporphyrin III dihydrochloride—a porphyrin produced by Propionibacterium acnes (Borelli, 2006).
PDT as means of acne treatments is especially exciting because P. acnes bacterium is a photosensitive microorganism. It naturally produces organic photosensitizers collectively known as porphyrins (Borelli, 2006). The primary porphyrin generated by P. acnes is Coproporphyrin III dihydrochloride (CIIID) (Borelli, 2006) (Figure 2). Even more enthusing is the fact that these molecules are present in high concentrations even under normal conditions. This is extremely beneficial for PDT treatment because the photosensitizers do not have to be injected or supplemented in any other way. Recent spectra analysis of CIIID’s absorption spectrum (process that measures a molecule’s absorption of light as a function of wavelength) has determined that 632.8nm (red light) and 405 nm (blue light) are the wavelengths in which significant absorption is exhibited (Thoreson, 2010). This means that 632.8nm and 405nm are the wavelengths of light that will react with CIIID and instigate the “domino effect” of the subsequent reactions that ensue. Thus, lasers that emit light of these wavelengths are a primary means of acne therapy. PDT continues to be increasingly employed in clinical dermatology. It has been an advantageous form of treatment because P. acnes produce its own porphyrins (CIIID), and because the effects of PDT occur only in targeted, illuminated cells. The distinctiveness of PDT is more pronounced in acne because no other known healthy cells in the skin create porphyrins. Furthermore, the eradication of bacteria through the application of visible (red and blue) light—as opposed to UV rays which would have unwanted adverse effects upon healthy as well as diseased cells—is tremendously beneficial. Although researchers persist in their confidence that PDT offers the best hope for controlling or eliminating acne, the specific mechanism by which emitted light eradicates the P. acnes along with the bacterium’s possible propensity for resistance has not been thoroughly analyzed. A consistent method of effectively and efficiently eradicating P. acnes by means of PDT is still undergoing research. In addition, the ways by which the photosensitivity of P. acnes can be increased are not fully understood. Hence, this research project specifically aims to isolate the best and most productive conditions for effective PDT eradication of P. acnes. This research lays out a series of appealing inquiries in regards to possible enhancement of P. acnes ’ photosensitivity by analyzing several factors in vitro (in a test tube, outside a living organism). The first factor that will be examined is the effect of the surrounding media (growth culture). Bacterial cells are grown in vitro in a liquid solution that contains all the necessary nutrients for the growth and sustenance of the microbe. PDT treatment of P. acnes cells within their growth culture may enhance the photodynamic effects because P. acnes cells continually produce CIIID within their growth media. Thus, there will, in theory, be an increased number of porphyrins able to absorb and transmit the light to the surrounding oxygen molecules. The second factor that will be examined is the effect of oxygenation. As oxygen molecules are the final acceptors of the energy transmitted from the porphyrins, an increased number of oxygen molecules should lead to an increase in the number of singlet oxygen formed, enhancing the eradication of bacterial cells. The third factor is the introduction of a solution of hydrogen peroxide (H2O2) and Iron tri-Chloride (FeCl3). Combining H2O2 and FeCl3 produces what is called a Haber-Weiss reaction that yields a superoxide radical and Iron III (Prousek, 2007). In a subsequent reaction, the superoxide radical (formed in the Haber-Weiss reaction) reduces (donates its electrons to) Iron III, resulting in the formation of Iron II. Iron II then initiates a Fenton reaction—a chemical reaction in which Iron II reacts with H2O2. The Fenton reaction then generates hydroxyl radicals—highly reactive and unstable molecules that have similar destructive effects as singlet oxygen. The rationale is that the production of hydroxyl radicals from the addition of H2O2 and FeCl3will work alongside the singlet oxygen generated to significantly enhance the effects of PDT. The fourth factor considered is the effect an increase in the length of time the P. acnes cells remain in their respective growth cultures has on their susceptibility. As P. acnes bacterial cells continue to produce CIIID, even when not actively growing, increased time within the growth media would allow for increased production of CIIID. This would then, in theory, enhance PDT by providing many more molecules capable of being “excited” and inducing the cascade of events that result in apoptosis or necrosis. Thus, the P. acnes strains tested for this factor were allowed to remain refrigerated in their growth media for a period of 4 months. Along with examining factors that may enhance photodynamic therapy, this research also examines whether P. acnes that have already undergone treatment with PDT become resistant when treated with PDT a second time. Antibiotics became ineffective means of acne treatment due to the rise of antibiotic resistant bacterial strains. Thus, this research examines whether these same issues will be present in photodynamic therapy. Overall, the purpose of this experiment is to determine if molecules in the surrounding growth media, oxygenation, H2O2 + FeCl3 supplementation, and bacterial storage in growth media for 4 months significantly enhance the susceptibility of P. acnes to photodynamic therapy. Moreover, this experiment also examines if the P. acnes strains that have already undergone photodynamic therapy become resistant when treated with PDT a second time.Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Biology |