Shedding New Light on Acne: The Effects of Photodynamic Therapy on Propionibacterium acnes
By
2013, Vol. 5 No. 09 | pg. 1/4 | »
IN THIS ARTICLE
KEYWORDS
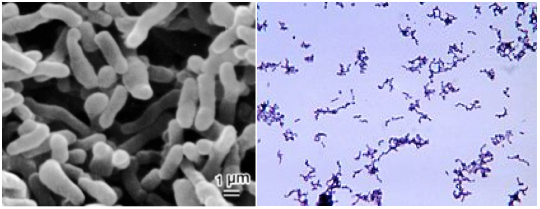
AbstractThe purpose of this experiment is to determine the susceptibility of propionibacterium acnes to photodynamic therapy (PDT). Propionibacterium acnes (P. acnes) is the leading cause of acne vulgaris—a chronic inflammatory skin disorder that affects an estimated 80% of Americans. Antibiotics are the primary means of acne treatment; however, the emergence of antibiotic resistant P. acnes has made it ineffective. PDT is an alternative form of treatment that excites P. acnes’ naturally produced photosensitizer, corporprophyrin III dihydrochloride (CIIID), and induces a cascade of events that eventually result in P. acnes’ cell death. This experiment determines if the effects of PDT can be enhanced by illuminating bacteria that are unwashed, oxygenated, H2O2 + FeCl3 supplemented, and stored for 4 months. It also examines if previously illuminated bacteria become resistant to PDT. All bacterial cultures were grown anaerobically in brucella media and illuminated with 632.8nm of light using Metrologic helium-neon laser. All the bacterial cells were significantly susceptible under all conditions (P<0.05, t-test). Unwashed, oxygenated, and bacteria that were stored for 4 months resulted in cell death of more than 25%. Previously illuminated bacteria were not significantly resistant when treated with PDT a second time (P>0.05). All in all, this experiment has generated results that fall within the expected effects of PDT. The various factors that have enhanced the effects of P. acnes susceptibility to PDT, and the lack of P. acnes resistance to secondary treatment of PDT, lead to more intriguing questions and warrant further in vitro and in vivo experimentation. Propionibacterium acnes (P. acnes) is the leading cause of acne vulgaris—a chronic inflammatory disorder of the skin (Perry et. al, 2006). Acne vulgaris, or simply acne, is a common skin disease that affects an estimated 80% of Americans at some point during their lives (Fulton, 2012). If heart disease, lung cancer, obesity or allergies were affecting 80% of any subset of the U.S. population, citizens would be issuing calls for action. However, acne’s ubiquity has in some ways numbed the public into mistakenly believing that like “bad-hair-days,” it is just something they have to cope with until it subsides. Furthermore, acne’s external symptoms have also led many to suppose that its effects are solely superficial—but that is not the case. While its most evident effects appear upon the surface of the skin, acne has also been shown to induce various psychological and psychosocial ailments. Acne is characterized by the appearance of seborrhea (scaly red skin), comedones (blackheads and whiteheads), papules (pinheads), pustules (pimples), nodules (large pinheads) and scarring (Bojar et. al, 2004). These symptoms generally decrease over time and tend to fade by around age 25, but there are no specialized ways to determine how long it will take for the symptoms to disappear entirely. Moreover, of all affected individuals in the U.S., twenty percent (48 million people) will have severe acne, which results in permanent scarring. Clearly, acne—constituting 30% of all dermatological visits in the United States each year (Elman, 2004)—is a prevalent dermatological issue.But the issues of acne surpass its dermatological effects. Recent studies have shown that the mental and emotional scarring that results from acne have led to a mounting poor self-image, depleted self-esteem, and in extreme cases, depression or suicide (Purvis, 2006). As acne commonly occurs during adolescence—when individuals already tend to be socially insecure—the psychological effects of acne are more pronounced in the youth. Teenagers with acne are at increased risk of depression, anxiety and suicide attempts (Purvis, 2006).Thus, acne should not be regarded as a mere cosmetic issue, but instead as an ailment that can underline and outlive its superficial effects. Process of Acne DevelopmentAlthough multifaceted lists of supplementary causes—both genetic and environmental—are also associated with acne, the decisive development of acne is attributed to the increased proliferation of Propionibacterium acnes (Jappe et. al, 2002). P. acnes is a bacterial species that subsists deep within the follicles (tissue around the root of hair) and pores of the skin. The bacterium derives its energy from sebum (oily secretions), cellular debris and metabolic byproducts from the surrounding tissue (Leyden, 2001). Interestingly, P. acnes is a microbe that in principle is commensal, meaning the bacterium benefits while the organism it infects derives neither benefit nor harm (Bruggemann, 2004). Thus it is present in the normal skin microbiota of healthy individuals. However, when present in excess, it will have the negative health effects associated with acne vulgaris. In this way, it is similar to fat, which is present and even necessary for leading a healthy lifestyle, but when found in excess results in obesity and its ensuing health defects. P. acnes is produced in excess as a result of several successive factors that proceed in a cascade of events. First, an increase in the production of androgens (sex hormones), which most notably occurs during puberty, stimulates the hyperactivity of sebaceous glands—microscopic glands responsible for the greasiness of the skin. Hyperactive sebaceous glands then augment the formation of sebum and keratin—a protein that is the main constituent of hair. Sebum and keratin in excess then make skin oily and clog pores, respectively. The pores, now clogged, accumulate dirt that would have otherwise been excreted, while the sebum creates an environment where P. acnes can flourish. Then the P. acnes secrete several proteins, including digestive enzymes, which allow for the absorption of sebum and the acquisition of other nutrients to further stimulate their growth. The proteins released by P. acnes also promote leukocyte (white blood cell) migration and follicular rupture. Subsequently, the numerous white bloods cells infiltrate around the hair follicles, triggering inflammation (Jappe et. al, 2002). The inflammation then leads to the destabilization of the layers of the cell that forms the wall of the skin, resulting in the various trademarks of acne such as pimples and blackheads. Characteristics of P. acnesCompared to those without acne, the number of P. acnes present in individuals with acne reveals a startling difference of 84,412 P. acnes organisms per square cm (Leyden, 2001). As a result, current studies on acne have focused on illustrating and expounding upon the physical and functional characteristics of P. acnes. Figure 1. Left- Rod shaped P. acnes seen through Scanning Electron Microscopy. Lines represent 1µm in length (Leyden, 2001). Right- Propionibacterium acnes grown in thioglycollate medium, stained with crystal violet. A 100x objective was used (Jappe et al., 2002).
P. acnes is gram-positive bacteria, which means it stains purple in Gram’s method—a staining technique used to distinguish between two categories of bacteria, positive and negative, based upon their ability to retain crystal violet (purple) or safranin (pink) dye, respectively (Figure 1). The bacterium is a facultative anaerobe—it has the advantageous ability to grow in both the presence and absence of Oxygen. Its cells are rod (football) shaped and are non-motile. It is a small bacterium approximately 0.5 µm wide and 1.5 µm long (Jappe et. al., 2002). Its small size is favorable—for both itself and the host cell—as it is found in significant amounts in extremely minute areas within the skin. Moreover, P. acnes is photosensitive; it reacts to light by absorbing photons (light particles) of specific wavelengths and transmitting the energy absorbed to surrounding molecules.Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Biology |