Shedding New Light on Acne: The Effects of Photodynamic Therapy on Propionibacterium acnes
By
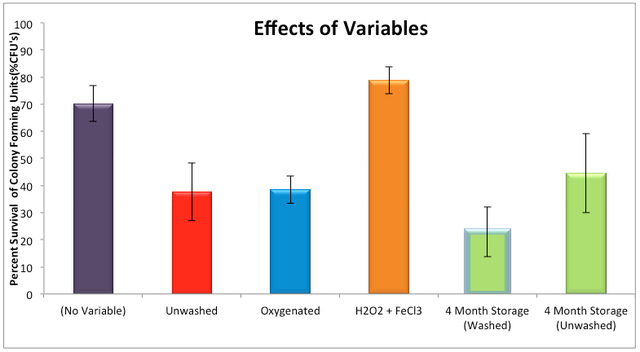
2013, Vol. 5 No. 09 | pg. 4/4 | « ResultsColony Morphology The colony morphology of NC, OC, RC and BC strains of P. acnes were circular, small and had a distinct cream color. The observable qualities of the colonies were consistent with literature. There were no contaminants present on any of the plates or culture tubes. Susceptibility of BacteriaWhen the New Culture (NC) bacterial cells were illuminated under normal conditions (no variable), the bacterial cells were susceptible to photodynamic therapy—there was a significant difference between the un-illuminated (100±0%, n=4) and illuminated NC bacteria (70.22±13.15%, n=4) (P=0.004,t-test, mean±SD)(Figure 3). NC bacterial cells illuminated under the unwashed (37.67± 21.2%, n=4) (P=0.001, t-test, mean±SD), Oxygenated 38.5± 10.1%, n=4) (P<0.0001, t-test, mean±SD), H2O2 + FeCl3 supplemented (78.89± 10.04%, n=4) (P=0.004, t-test, mean±SD), and 4 month storage for both washed (22.8± 18.34, n=4) (P=0.001, t-test, mean±SD) and unwashed (44.57± 29.12, t-test, mean±SD) conditions (P=0.009) were all significantly susceptible when compared to their respective un-illuminated controls (100±0%, n=4). The average percent survival colony forming units (22.8±18.34) of NC bacterial cells that were stored for 4 months and washed was the lowest of all variables. The percent survival of the “4 month stored” washed NC bacterial cells was significantly lower than NC bacterial cells under normal and H2O2 + FeCl3 conditions (P<0.01, t-test). However, the values did not significantly differ from the oxygenated, unwashed, or the “4 month stored” unwashed bacterial cells (P>0.2, t-test).
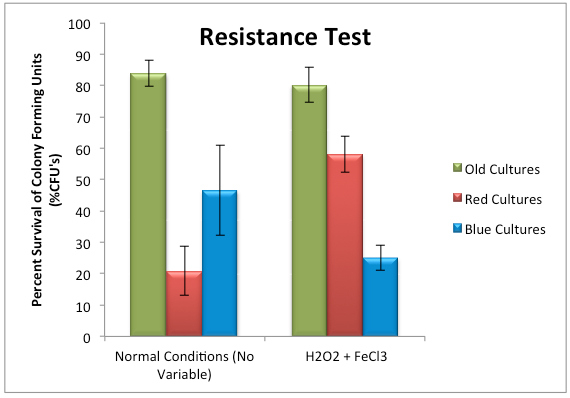
Propensity for Resistance The previously red light (RC) and blue light (BC) illuminated P. acnes strains did not exhibit any resistance to secondary treatment with PDT under any of the variables. In contrast, under normal conditions (no variable), the bacteria previously illuminated with red light, RC (20.84±14.6%, n=4), was found to be significantly more susceptible to PDT than the bacterial strain that had never been illuminated (83.77±8.31%, n=4)(p=0.01, t-test, mean±SD) (Figure ). Under the H2O2 + FeCl3 variable, the bacteria that was illuminated with blue light in a previous experiment, BC (25.09±6.2%, n=2), was found to be significantly more susceptible to PDT than the bacterial strain that received no prior treatment (80.2±5.67%,n=2)(P=0.01, t-test, mean±SD) (Figure 4). Figure 4. Percent Survival of Colony Forming Units following red light illumination of Old Cultures, Red Survivors, and Blue Survivors under Normal (No variable) and H2O2 + FeCl3 conditions. Error bars depict Standard Deviation. * indicates significant difference (P<0.05).
DiscussionOverall, this experiment supports that P. acnes are significantly susceptible to PDT—i.e., they die in considerable amounts when exposed to red light (632.8nm), even under normal conditions (no variable). Determining this feat was essential prior to even analyzing any other modes of enhancing these effects because the theory underlying PDT is its ability to penetrate into P. acnes cells and excite the porphyrin CIIID. Since CIIID is present in P. acnes all the time, PDT should have been able to exert its effects without the input of any outside influences—and that was the case here. While all strains of the bacteria under all variables were significantly susceptible to PDT, P. acnes responded differently to the various factors they were exposed to. The findings concerning the various factors that affect P. acne susceptibility are what are new to the study of PDT as a whole. In this experiment, we first studied the ways by which PDT exerts its effects and then attempted to enhance those effects by manipulating some of the systematic changes involved in the processes. The first factor that was tested was that of “unwashed” bacteria. This factor was intriguing because of the possibly increased number of CIIID that would be present in the surrounding media of the unwashed bacteria. Since PDT kills cells by exciting porphyrins and causing a “domino effect,” the rationale here was to see if increasing the number of available porphyrins for light to hit would increase this “domino effect.” According to findings from this experiment, that is exactly the case. On average, there were 33.34% more unwashed bacterial colony forming units (CFU’s) killed compared to the normal, no variable, conditions. This means attacking the bacterial cells in their growth environments, without isolating the cells themselves, will have increased efficacy. This finding is extremely fascinating because in the skin, the bacterial cells are found in their normal growth environments. At the onset of PDT treatment, there was concern that for PDT to exert its effects more pronouncedly, it would have to penetrate isolated bacterial cells. However, the results of this experiment indicate that the growth environment of the bacterial cells considerably intensify (not hinder) the effects of PDT. The second factor tested was oxygenation. As oxygen molecules are the final acceptors of the energy transmitted from porphyrins, an increased number of oxygen molecules should have led to an increase in bacterial susceptibility—and that, again, was the case here. Saturating the bacterial cells with oxygen prior to illumination resulted in 32% more deaths than the normal (no variable) conditions. This is remarkable because not only does shed more light on the processes of PDT, but it also provides new ways of tackling the problem of acne with PDT. Exposure of tissue to Oxygen molecules just prior to PDT treatment could result in a significant decrease of acne in vivo (in living organisms). And because porphyrins only transmit their energy to molecules that are in close proximity, there would (in theory) not be any adverse effects to healthy cells and tissues in other parts of the body. There are still other factors that need to be studied in regards to oxygenation and PDT but this finding offers a wide range of possibilities for future research—it opens the door for numerous other experiments concerning duration, amount and level of oxygenation. The possibilities are almost endless, and they are exciting. The third factor examined was the introduction of H2O2 and FeCl3. The toxic radicals formed from the reaction between H2O2 and Iron tri-Chloride were expected to work alongside the singlet oxygen generated from the normal effects of PDT to enhance susceptibility, but that was not the case. In fact, bacterial cells supplemented with H2O2 + FeCl3 were even less susceptible than bacterial cells illuminated under normal (no variable) conditions. On average 8% more bacterial cells with H2O2 + FeCl3 that survived illumination. These results were not anticipated (nor desired). However, the findings still shed light on the processes that occur in photodynamic therapy. Radicals are highly reactive and very unstable—they are reactive towards other substances in close proximity. By trying to increase the amount of radicals present, there’s a chance that we actually provided a means by which the toxicity of the radicals could abate. The hydroxyl radical produced may have potentially reacted with the singlet oxygen molecule, offsetting the toxic effects of both the hydroxyl and singlet oxygen radicals and rendering cell death by means of PDT ineffective. While the aim of applying this factor was to enhance the effective kill rate of the bacterial cells by PDT, it did act in accordance. However, the decreased susceptibility in the presence of H2O2 + FeCl3 does not hinder the effects of PDT by any means. This is because of the other factors that have significantly contributed to an enhanced kill rate, and because introducing H2O2 + FeCl3 in vivo could have possibly had adverse effects outside the scope of acne treatment. The fourth factor considered was the effect an increase in the length of time the P. acnes cells remain in their respective growth cultures has on their susceptibility. The rationale behind integrating this test is similar to that of the “unwashed” variable. As P. acnes bacterial cells continue to produce CIIID, even when not actively growing, increased time within the growth media would have allowed for increased production of CIIID. This would have then, in theory, enhanced PDT by providing more molecules capable of being “excited” and inducing the cascade of events that result in apoptosis or necrosis of P. acnes cells—and that was the case here. The bacterial cells stored for a period of 4 months and washed were on average 47% more susceptible than the bacterial cells that were illuminated under normal (no variable) conditions. This was by far the most pronounced enhancement of any of the variables. The “4 month stored” bacterial cells that were left unwashed were also more susceptible with an average of 25% bacterial cells killed compared to bacteria illuminated under normal conditions. This finding is intriguing because, like the “unwashed” bacterial cells, it indicates that leaving the bacterial cells in their normal growth environments with their surrounding molecules increases their susceptibility. On a broader scale, this approach leads to a possible means of acne treatment without the isolation of the particular bacterial cells. If this finding could be repeated in vivo, it would allow for a much easier and more accessible means of acne treatment. Along with examining factors that may enhance photodynamic therapy, this research also examined whether P. acnes bacterial cells that have already undergone treatment with PDT would become resistant when treated a second time. Resistance to treatment had been the problem with using antibiotics; thus, it was essential to examine whether these same issues would be present in PDT. The results of this experiment indicate that P. acnes do not become resistant to PDT treatment at any time during their lifespan. None of the bacterial strains exhibited any form of significant resistance to any of the variables they were exposed to. In fact, those bacterial cells that were previously illuminated with red light were found to be even more susceptible than the bacterial cells that had never been illuminated under normal conditions. Furthermore, bacterial cells that had previously undergone blue light illumination were found to be more susceptible to PDT under the H2O2 + FeCl3 variable. This finding was unexpected, yet remarkable. Antibiotics became an ineffective means of acne treatment due to the rise of antibiotic-resistant bacterial strains. Antibiotic resistance is a serious and growing phenomenon that has become eminent in 21st century medicine. Resistance is generated through the acquisition of a genetic mutation within the bacterial genome. However, in the case of PDT, the bacterial strains appear to not acquire such mutations and alter the components of their porphyrin CIIID. Further studies, possibly illuminating bacteria a third, fourth or fifth time, is necessary in order ascertain that the bacteria do not become resistance at any point during their lifespan. If the findings of this experiment are supported by other such studies, our findings may even lead to the consideration of PDT as a form of treatment for other ailments that have been limited with microbial resistance. All in all, this experiment has generated results that are in conjunction with previously held perceptions of the processes of photodynamic therapy. Furthermore, the various factors that have enhanced the effects of P. acnes susceptibility to PDT lead to more intriguing questions and warrant further studies applicable both in vitro and in vivo. The lack of bacterial resistance to PDT is extremely beneficial because microbial resistance has been an eminent glitch in 21st century medicine. Building on the findings of this experiment will lead to advancement in the effective treatment of acne vulgaris, so that people will no longer have to cope with acne as they do their “bad-hair-days.” Any reduction in the 80% of Americans suffering from acne is valuable. A problem cannot be fixed until people isolate and assess. Acne affects 240 million Americans and causes physical as well as mental scars—by any measure it is a significant problem. Accordingly, the findings of this experiment have supported previous studies that have and continue to endeavor to eliminate this “skin-deep” ailment. References"Acne Cystic Photo - Skin Disease Pictures."Dermnet.com. Dermnet, 13 Mar. 2011. Web. 12 Mar. 2013. Bojar, Richard A., and Keith T. Holland. "Acne and Propionibacterium Acnes."Clinics in Dermatology22.5 (2004): 375-79. Print. Borelli, C., K. Merk, M. Schaller, K. Jacob, M. Vogeser, G. Weindl, U. Berger, and G. Plewig. "In Vivo Porphyrin Production by P. Acnes in Untreated Acne Patients and Its Modulation byAcne Treatment."Acta Dermato-Venereologica86.4 (2006): 316-19. Print. DeLaney, Thomas F., and Eli Glatstein. "Photodynamic Therapy: Theory and Practice."International Journal of Radiation OncologyBiologyPhysics21 (1991): 84. Print. Elman, Monica, and Joseph Lebzelter. "Light Therapy in the Treatment of Acne Vulgaris."Dermatologic Surgery30.2 (2004): 139-46. Print. Fulton, James, MD. "Acne Vulgaris - Overview."Emedicine.medscape.com. WebMD LLC., 28 June 2012. Web. 7 Oct. 2012. Harth, Yoram. "Comedones And Acne Pimples: How They Develop ?"Skintricks.com. Rational Mind LTD, 11 Sept. 2010. Web. 12 Mar. 2013. Jappe, U., E. Ingham, J. Henwood, and K.T. Holland. "Propionibacterium Acnes and Inflammation in Acne; P. Acnes Has T-cell Mitogenic Activity."British Journal of Dermatology146.2 (2002): 202-09. Print. Jemec, Gregor B.E., and Barbara Jemec. "Acne: Treatment of Scars."Clinics in Dermatology22.5 (2004): 434-38. Print. Leeper, F. J. "The Biosynthesis of Porphyrins, Chlorophylls, and Vitamin B12."Natural Product Reports2.6 (1985): 561. Print. Leyden, J. "The Evolving Role of Propionibacterium Acnes in Acne."Seminars in Cutaneous Medicine and Surgery20.3 (2001): 139-43. Print. Midgley, M. "The Interaction of Oxygen with Propionibacterium Acnes."FEMS Microbiology Letters23.2-3 (1984): 183-86. Print. Perry, A.L., and P.A. Lambert. "Propionibacterium Acnes."Letters in Applied Microbiology42.3 (2006): 185-88. Print. "Pimples and Circumstance."ScienceSavvy. N.p., 13 Oct. 2012. Web. 12 Mar. 2013. Prousek, Josef. "Fenton Chemistry in Biology and Medicine."Pure and Applied Chemistry79.12 (2007): 2325-338. Print. Purvis, Diana, Elizabeth Robinson, Sally Merry, and Peter Watson. "Acne, Anxiety, Depression and Suicide in Teenagers: A Cross-sectional Survey of New Zealand Secondary School Students."Journal of Paediatrics and Child Health42.12 (2006): 793-96. Print. Thoreson, Anders J., John W. Kenney III, and Michael E. Young. "Synergistic Effects of Spectral Conditions and Photodynamic Therapyon Coproporphyrin III Dihydrochloride Produced by Propionibacterium Acnes Responsible for Acne Vulgaris." (2010): n. pag. Web. Torpy, J. M. "Acne."JAMA: The Journal of the American Medical Association292.6 (2004): 764. Print. Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Biology |