From Discussions VOL. 11 NO. 2Does BMI Affect Diagnostic Efficacy of Computer Aided Diagnostic Software in the Identification of Malignant Pulmonary Nodules in Dual Energy Subtracted Chest Radiographs?
IN THIS ARTICLE
KEYWORDS
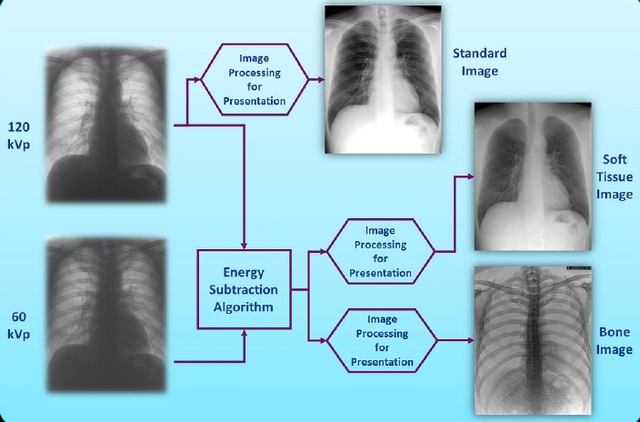
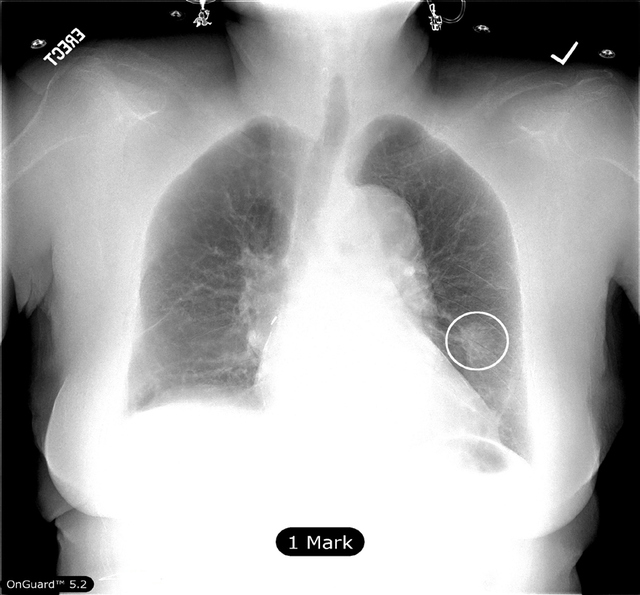
AbstractThe increasing level of obesity in the general population of industrialized nations is a major public health concern. While obesity increases morbidity and mortality, increasing body habitus also impacts the utilization and analysis of medical imaging. The purpose of this retrospective pilot study is to compare the diagnostic effectiveness of Computer Aided Diagnosis (CAD) software (OnGuard™ 5.2) in combination with a hardware based bone suppression tool, Dual Energy Subtraction (DES) radiography on thoracic radiographs of patients with varying levels of obesity. Chest radiographs from 30 patients with CT and pathology verified malignant pulmonary nodules (8-34 mm) and 23 CT negative patient controls with different levels of obesity as measured by Body Mass Index (BMI) were utilized for analysis. Twentysix patients had a normal BMI (18.5-25) and twenty-seven patients were overweight, obese or morbidly obese (OOMO) with a larger BMI value (between 25-47). Test Sensitivity and Specificity, Analysis of Variance (ANOVA), Z-test for Equality of Proportions, Spearman’s rank correlation coefficient and the independent sample Student’s t-test were calculated. P-values less than 0.05 were considered significant. Age was not significantly different between the two BMI groups (t=1.26, p=0.26). CAD software Sensitivity =80.0% and Specificity=72.7% in normal BMI patients while for OOMO patients, Sensitivity=83.3% but Specificity was reduced to 44.4%. The difference in Specificity between the Normal and OOMO patients approached significance (p=0.09) using the one tailed equality of proportions test (Z=-1.3). Similarly, in normal patients, BMI and the number of Regions of Interest (ROI) were nearly significantly correlated (ρ=0.374, p=0.06) while there was no significant correlation between BMI and ROI for OOMO patients, (p>0.5). There was no difference in Sensitivity between the Normal and OOMO groups; however there was likely a clinically significant difference in Specificity between the two groups, if not a statistically significant difference. Obesity appears to cloud the ability of CAD to identify the absence of malignant pulmonary nodules in OOMO patients. A study with a larger number of patients, particularly obese and morbidly obese patients, may provide a more accurate view of this discrepancy. IntroductionChest radiography is one of the most commonly used forms of radiologic examination. One of the goals of chest radiography is the identification of malignant pulmonary nodules. Several authors have suggested that Computer Aided Detection (CAD) may help radiologists to detect cancerous pulmonary nodules (Li, Engelmann, Metz, Doi, & MacMahon, 2008; Oda et al., 2009). CAD identifies Regions of Interest (ROI) on chest radiographs as areas suspected to be malignant. These ROI are identified as circles imposed on the radiograph. However, high numbers of false positives identified by early versions of CAD software on standard postero-anterior (PA) chest images limited the clinical utility of this technology (Bley et al., 2008; Kasai, Li, Shiraishi, & Doi, 2008; Kobayashi, Xu, MacMahon, Metz, & Doi, 1996). Meziane et al. (2011) indicated that CAD software improved recall rates and diagnostic accuracy, particularly in cases with small pulmonary nodules or inexperienced readers. Other researchers (Monnier-Cholley, Carrat, Cholley, Tubiana, & Arrive, 2004; Shah et al., 2003) determined that a large proportion of the false positives and missed lung cancer cases occurred because of bony structures in the chest, in particular clavicles and rib crossings. The literature on the subject suggests that the use of bone suppression improves the diagnostic accuracy of digital chest radiography. Many authors advocate the suppression of ribs and clavicles in digital chest images to improve malignant nodule detection by (CAD) software. Currently, several methods exist to suppress bone and other calcified structures in digital chest radiographs. One method is hardware-based, Dual Energy Subtraction (DES) radiography (GE Healthcare). Oda et al. (2009) determined that the use of DES radiography significantly improved the radiologists’ diagnostic performance in detecting ROI. Other studies found that hardware based bone suppression (DES) removed the presence of bony structures in digital chest radiographs and significantly improved the sensitivity of CAD, which reduced the false-positive diagnosis rate (Balkman, Mehandru, DuPont, Novak, & Gilkeson, 2010; Li et al., 2011; Szucs-Farkas, Patak, Yuksel-Hatz, Ruder, & Vock, 2010). Unfortunately, body fat attenuation of the x-ray beam used in thoracic radiography causes reduced image contrast and increased image noise that may lead to variance in the diagnostic performance of CAD software. These studies suggest that CAD together with bonesuppressed images improves the diagnostic accuracy of pulmonary nodule detection. Yet, the role of obesity in CAD efficacy has not been investigated despite the fact that the Centers for Disease Control notes that roughly two thirds of all Americans are overweight and over half of them are classified as obese (Buckley et al., 2009). Obesity is measured by Body Mass Index (BMI) which is defined as mass in kilograms divided by the square of height in meters (kg/m2). Obesity has many serious short and longterm health effects that increase the risk of early morbidity and mortality including hypertension, diabetes, heart disease and cancer. Beyond these risks, obesity also creates difficulty with diagnostic imaging procedures and test interpretation. Several studies have concluded that obesity (BMI > 30) and particularly morbid obesity (BMI > 40) affects not only the quality of medical imaging (Reynolds, 2011; Uppot, 2007) but also the ability to use some imaging methods because patients are inhibited from using equipment designed for individuals of normal weight (Twaij, Sodergren, Pucher, Batrick, & Purkayastha, 2013; Uppot, 2007). Further, extreme obesity has been found to adversely affect the ability to interpret the results of radiological examinations (Larson, Franzblau, Lewin, Goodman, & Antao, 2014; Rajapakse & Chang, 2014). Increased levels of obesity make diagnostic determination of physiological landmarks more difficult (Ambardar et al., 2009), but also make the results of other imaging procedures less accurate (Carboni, Sedati, & De Marco, 2013; Twaij et al., 2013). The purpose of this study was to compare the diagnostic effectiveness of CAD+DES bone suppression software combination to detect malignant pulmonary nodules when used on patients with differing levels of obesity as measured by BMI. As stated earlier, increased numbers of false positives (FP) and false negatives (FN) reduce the diagnostic efficacy and utility of CAD products in diagnostic radiology. The hypothesis of this study is that increasing levels of obesity alter the diagnostic efficacy and the number of ROI and FP marked by CAD. MethodsInstitutional review board approval was obtained from University Hospitals Case Medical Center for this project. The approval for informed patient consent was waived and patient records were handled in compliance with Health Insurance Portability Accountability Act (HIPAA) regulations. All patient images and records were maintained on encrypted storage devices to maintain HIPAA compliance. Patient SelectionMedical records and images from University Hospitals Case Medical Center were reviewed and sixty patients with either pulmonary nodules confirmed by 16 or 64 slice computed tomography (CT) and pathology verified lung carcinoma were selected. Individuals with single lung nodules 8-34 mm in size were selected as this size range is most likely to be missed by a radiologist. The nodules were located in a variety of locations in the lungs. This sample included 30 patients with CT and pathology proven malignant nodules and 23 patients without malignant nodules as determined by 16 or 64 slice CT. In individuals with malignant nodules, the size and location were measured and marked on standard Posteroanterior (PA) radiograph by an expert radiologist with 24 years of experience. Patient records were reviewed for height and weight, gender and age. Patients were divided into obesity groups by BMI and classified as: Normal (BMI=18.5-25), Overweight (BMI= 25-30), Obese (BMI=30-40) and Morbidly Obese (BMI=40+). Underweight individuals (BMI < 18.5) were omitted from the analysis. Due to the small sample size, two groups were formed; normal individuals (18.5 Soft Tissue Image and CAD Software AnalysisDES radiography , one form of bone suppressed image generation, was performed on a Revolution XRd/ Definium™ digital radiography unit (General Electric Medical Systems). This radiography unit consisted of a 41 x 41 cm2 amorphous silicon based flat panel detector. DES radiography is performed using the acquisition of a low energy 60 kVp PA chest radiograph taken after a 150 ms delay, and a high energy 120 kVp radiograph. Subtracted and bone-enhanced images are also presented after postprocessing of the high and low energy radiographs as depicted in Figure 1. Bone Suppression and CAD SoftwareOnGuard™ Computer Aided Diagnostic (CAD) software was used to identify potential ROI that may be identified as malignant nodules. The stand-alone version of CAD software known as OnGuard™ (Riverain Technologies, Miamisburg, Ohio, USA) was utilized for this study as OnGuard, Version 5.2. Unlike previous versions, OnGuard™ Ver. 5.2 incorporated an additional bone suppression algorithm to better identify areas of interest prior to applying the CAD markings to the radiograph. The CAD component of the OnGuard™ CAD system identified ROI by imposing circular markings on the radiographs. Examples of CAD markings on a bone suppressed DES image is shown in Figure 2. The circular marks were centered about a detection location that signified the identification of a probable malignant nodule. For identification of true positive detection and sensitivity, the known central point of the known nodule location must have been enclosed by the circular marking method of the CAD software and greater than 50% of the radiologist outlined nodule must have been also enclosed by the CAD mark. All other ROIs were determined to be false positives including those generated on CT proven negative cases. Figure 3 depicts true positive and false positive example markings on a bone suppressed DES image. Statistical AnalysisSPSS Version 21 statistical software (IBM Corp, Armonk, NY) was used for statistical calculations. Correlation between several variables and ROI and FP frequency were evaluated by using the Spearman Rank Correlation test, chosen because of the non-normal distribution of ROI and FP. Test sensitivity and specificity were calculated using standard methods, Analysis of Variance (ANOVA), Chi-Square, the Z-test for Equality of Proportions and the independent sample Student’s t-test were calculated to identify statistically significant differences between BMI groups. P-values less than 0.05 were considered significant.Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Biology |