From Discussions VOL. 5 NO. 2Development of a Micro-integration Technique for the Fabrication of a Cell-Fiber Scaffold Complex in Heart Valve Tissue Engineering
IN THIS ARTICLE
KEYWORDS
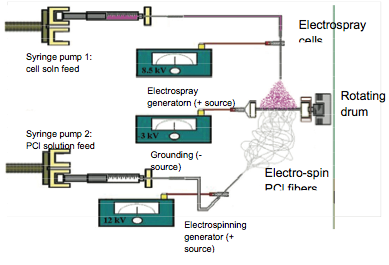
AbstractAll clinically available heart valve prostheses, such as mechanical and bioprosthetic valves, are intrinsically flawed in that they are unable to grow and become a fully functional part of the native tissue. In response to this critical need for a better heart valve substitute, we aim to develop a multifunctional scaffold that ideally mimics a native heart valve in mechanical properties, serves as a growth factor and cytokine delivery vehicle, and supports cell attachment and proliferation through tissue engineering. An innovative technique known as micro-integration, involving simultaneous electrospraying of cells and electro-spinning of fiber matrix, is designed and optimized for uniform and selective positioning of cells within a scaffold. The effectiveness of this process, as well as cell viability, proliferation and location in scaffold are then assessed using live/dead cell assay and fluorescence and confocal microscopies. Preliminary work involves electrostatic spraying of fluorescent NIH 3T3 fibroblasts, endothelial progenitor cells and, eventually, mesenchymal stem cell into a polymer scaffold made from solutions of biodegradable and biocompatible polymers such as poly-(ε-caprolactone) in chloroform. Optical and scanning microscopy images of a seeded scaffold fixed in paraformaldehyde indicate improved cell growth and adhesion on fibrous surfaces with small pores in comparison to a smooth film of the same polymer. Fluorescent imaging shows uniform cell distribution throughout the scaffold. Unfixed portions of the scaffold cultured for subsequent assessment illustrate approximately 80% cell viability and growth via cell counting and live/dead stain. Future work will focus on improving the scaffold through controlled delivery of key growth factors and ensuring adequate nutrient and waste transport through controlled porosity. The expected outcome of this work is a state-of-the-art methodology for tissue engineering scaffold optimization which will lay a strong foundation for achieving the long term goal of developing a fully functional regenerated heart valve. IntroductionThe study of heart valve disease is an emerging area of research made possible by the design of in vitro and in vivo cellular experimental involved in development of synthetic valves. Heart valve disease is a health care concern that draws much attention in society as it affects a significant portion of the international population. Every year, about 5 million Americans learn they have heart valve disease (Nkomo et al., 2006). The common treatment of end stage valvular disease is valve replacement, followed by prosthetic valve implantation. Currently, the two types of prosthetic valves available— mechanical and synthetic valves—are both flawed. A principal limitation of the use of mechanical prosthetic valves is the need for a life-long anticoagulation to treat thromboembolism. While synthetic valves do not require continuous anticoagulant use, they are only durable for 10 to 15 years due to matrix calcification, which requires frequent reoperation. The operation-associated complications increase patients' morbidity, mortality and financial burdens. Furthermore, the fact that all clinically available heart valve prostheses cannot grow and function fully as part of the native tissue is a particular concern in pediatric patients who are still growing (Fong, Shin'oka and LopezSoler, 2006). Clearly, there is an urgent need for an improved heart valve substitute, which can be accomplished through the use of tissue engineering and regeneration. The advantage of investigating synthetic scaffolds is that they allow for controlled development of valve mechanical properties and varied matrix structure obtained from different types of polymers. Tissue engineered scaffolds act as a template for complex heart valve construct re-growth. Ideally, scaffolds should facilitate cell attachment and proliferation, provide an advantageous biochemical environment, and enable adequate nutrient and waste transport. Types of polymers available for fabricating scaffolds include poly(lactic acid), poly(glycolic acid), poly(lactic-co-glycolic acid),and poly(caprolactone). More commonly, a combination of these biocompatible and biodegradable materials is used. However, the rigid nature of the polyesters prevents the scaffolds from having similar mechanical properties and an architecture as complexly layered as the native leaflet. Many synthetic matrices also limit cell adhesion and scaffold infiltration (Mendelson and Schoen, 2006). Thus, scaffold development for heart valve tissue engineering needs improvements in both mechanical and cellular components. The long term goal of this work focuses on developing a multifunctional scaffold that: 1) possesses mechanical properties that meet the tissue engineering application requirements, 2) serves as a controlled multiple growth factor and cytokine delivery vehicle, 3) is capable of supporting cell attachment and proliferation and 4) influences progenitor cell differentiation through both physical and biochemical stimuli. This will be accomplished through a multidisciplinary approach involving the following: mathematical modeling and experimental design of biopolymer scaffolds with targeted mechanical properties and degradation rate, development of a controlled growth factor delivery model, and an innovative electrospraying-electro-spinning methodology (known as micro-integration) of cell incorporation into the biologically active scaffold. The immediate aim of the work presented in this paper is to enable selective distribution of endothelial cells and fibroblasts throughout the scaffold matrix via the micro-integration method, and to promote and assess cell viability and proliferation within the scaffold using fluorescence and optical microscopy. Histological staining and protein expression are used to evaluate the biological impact of the scaffolds with and without incorporated growth factor release. The electro-spinning technique is capable of producing microor nanofibrous scaffolds with similar morphological characteristics to natural extracellular matrices (Bowlin et al., 2002). It is a means of polymer processing making use of electric forces to form small diameter polymer fibers and non-woven mats of those fibers. In practice, the polymer solution loaded in a syringe is charged by a strong electrical potential to the metal needle, which is in the presence of a grounded target located on a rotating metal a few centimeters away. The application of the potential results in a charged jet of the polymer solution being released from the tip of the needle in the formation of a tailor cone. The jet travels through the air to a grounded collecting drum, leaving a solid polymer fiber. As fibers start to collect with time, a mat is formed. The jet diameter is usually a small fraction of that of the needle, and the resulting fiber diameters and pore sizes can vary depending upon the polymer flow rate and the distance between the tip of the needle and the grounded target. In the electrospraying process, drops of cells dispersed in cell media shoot out from the tip of another needle toward the same drum upon being charged by the electrical potential. Thus, the electro-sprayed cells are entrapped within the selected areas of the fibrous matrix in the formation of the cell-fiber construct. MethodsCell Selection and CulturePreliminary studies involved seeding GFP+ (green fluorescent) 3T3 fibroblasts into poly-(caprolactone) (PCl) scaffolds. GFP+ fibroblasts were chosen for the convenience of fluorescence spotting in optical imaging. Later experiments involved the use of endothelial progenitor cell (EPC) derived from umbilical cord blood, CD133+. This cell type is closest in replicating the natural cellular component found in the native leaflet tissue. To obtain these cells, mononuclear stem cells (MNSCs) were first isolated from samples of cord blood by conventional centrifuge methods through a Ficoll-density gradient. Whole blood samples were placed on top of Ficoll and then were centrifuged at 1,500 rmp for 30 minutes with the break open. Before isolation and seven days of culturing, recovered MNSCs were sucked and removed from the tube and placed into a new centrifuging tube containing phosphate-buffered saline (PBS). The culture media used was Medium-199, supplemented with 20% fetal bovine serum (FBS) and antibiotics. During this period, cell maturing and proliferation was induced. Flow cytometry was then used to identify the CD133+. In preparation for the microintegration process, the cells were detached using 0.05% trypsin from the flasks, where they were suspended in Medium-199 and DMEM, respectively, with 10% FBS. Then, cells were counted and placed in a sterile 5 mL syringe. Micro-integration ProcessPCl served as a starting point for our material investigation. A 12 wt% solution of PCl in chloroform was loaded in a 5 mL syringe with a blunt tipped 18 gauge stainless steel needle and horizontally positioned with respect to a sterilized, rotating metal drum with a surface area of 12.5 cm2. A second syringe containing approximately 4 x 106 fibroblasts in 0.6 mL culture media was positioned vertically above the collecting drum. A positive 15 kV voltage was applied to both syringes. In order to enhance fiber collection via opposite polarity, a negative 3kV voltage was applied to the drum instead of grounded. The electro-spinning flow rate was set at 1 mL/hr with the syringe positioned 0.8cm away from the target. The flow rate for electrostatic spraying process was 0.3mL/hr, and the syringe containing cells was placed at 0.4cm away from the target. Then, electro-spinning of the polymer and electrospraying of the cells were carried out simultaneously, as shown in Figure 1. The scaffold was allowed to build up to approximately 100 μm in thickness and then removed from the drum. A portion of the scaffold was removed, placed in growth media and kept in an incubator (37°C and 5% CO2). The remaining scaffold was fixed in paraformadehyde for imaging using optical and fluorescent microscopy. Figure 1: Experimental design of micro-integration set-up involving simultaneous electrospraying of cells and electrospinning polymer.
Later experiments focused on developing scaffolds consisting of multiple cell types and polymers. This was accomplished using a sequential approach to construct and form various layers. Outer layers consisting of collagen electrospun from hexafluoroisopropanol (HFIP) were combined with electrosprayed EPCs. These collagen layers were sandwiched around an inner layer of electrospun PCl containing electrosprayed mesenchymal stem cells. This allowed for the development of a scaffold consisting of two localized cell populations in a layered multi-component polymeric scaffold. Once constructed, the mats were kept in culture conditions with DMEM media with 2% fetal bovine serum. Electrospun mats were then characterized via scanning electron microscopy for fiber diameters and porosity. Cell distribution within the scaffold was identified through hematoxylin and eosin staining and visualized with light microscopy. Cell viability was also assessed using the dead/alive assay.Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |