From Discussions VOL. 4 NO. 1The Natural History of Osteoarthritis
IN THIS ARTICLE
KEYWORDS
Keywords:Osteoarthritis Hamann-Todd Collection
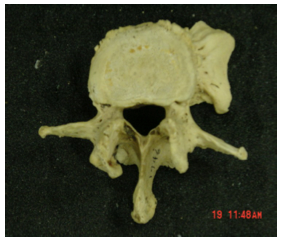
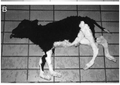
AbstractEarly signs of vertebral osteoarthritis begin to appear around the age of thirty. By age fifty, almost everyone exhibits some form of osteoarthritis in their spine, and with time the arthritis advances. The examination of a 3.2 million year-old ancestor verifies osteoarthritis‟ longstanding condition in bipeds. Osteoarthritis in the vertebral column is characterized by osteophyte formation, or "lipping," on any part of the vertebra (Nordin 1989). This comparative study aims to target the location, frequency, and severity of osteophyte formation in the thoracic and lumbar vertebrae of humans as well as the nonhuman primates. Each specimen was taken from The Hamann-Todd Osteological Collection at the Cleveland Museum of Natural History. The human sample comprises 89 specimens and the nonhuman sample 33. Each human and nonhuman specimen was closely examined in an effort to examine a potential relationship between the presence or absence of osteoarthritis in the flexible spinal column of the bipedal human and the largely immobile spinal column of the quadrupedal African apes. INTRODUCTIONOsteoarthritis (OA), also known as degenerative joint disease, is a condition resulting from progressive erosion of joint cartilage. As a result of this progressive degeneration lesions begin to form (Aufderheide 1998). OA can be seen in numerous joints throughout the body, such as the knee, hip, shoulder, elbow and spine. OA of the spine, also known as spondylosis, can be extremely debilitating. OA is manifested by lesions that are called "osteophytes," which are outgrowths of new bone (See Fig-1). In extreme cases this growth of new bone can lead to the fusion of two adjoining vertebrae (See Fig-1). In humans, range of motion and other movements such as rotation, flexion, and extension can be significantly decreased. If the fusion of two adjoining vertebrae occurs, adjacent vertebral bodies are at greater risk for OA. This stems from the adjacent vertebral bodies compensating for motion restricted in the fused vertebrae. If any movement at any level of the spine is restricted, the spine in turn will counteract by increasing motion at another level (Nordin 1989). Few mammals possess the spinal flexibility of humans. For example, African apes such as gorillas (Gorilla gorilla), and chimpanzees (Pan troglodyte), have a stiff, inflexible spine as an adaptation to large bodied arboreality. Anatomically, the apes have decreased the number of lumbar vertebrae to three or four, as opposed to five, the condition most common in the human lumbar spine. The apes also have increased the height of the iliac blades. These two evolutionarily selected characteristics have stiffened the ape‟s spine to strictly support bridging and climbing. As a result, apes have severely comprised the mobility of their spines. Although chimps and humans are phylogenetically very close, their vertebral columns differ dramatically. In contrast to the inflexible ape spine, humans possess an extremely flexible vertebral column. The extremely flexible nature of the human spine is a byproduct of our bipedal locomotion. The lumbar columns of early hominids such as Homo erectus and Australopithecus were comprised of six lumbar vertebrae, as opposed to the five vertebrae of modern Homo sapiens. The necessity of six lumbar vertebrae is derived from early hominids‟ attempt to move the last thoracic vertebrae T13 into a lumbar element, thereby increasing spinal mobility and the ability to balance their torso over the hip joints (Latimer 1993). Habitual bipedality has promoted mechanical demands not seen in the quadruped. These mechanical demands have rendered alterations of vertebral curvatures. Among mammals only humans and our immediate ancestors‟ genus Homo and Australopithecus posses sinuous curves which cauterize the bipedal spine. These curvatures are comprised of an anteriorly directed kyphotic curve in the twelve thoracic vertebrae, and a posteriorly directed lordotic curve in the lumbar vertebrae. The reason for this peculiar anatomy is to balance and distribute loading over the hips during locomotion (Latimer 1993). This comparative study examined whether the degeneration caused by OA is unique in humans due its evolutionarily selected mobile spine. We examined the flexible vertebral columns of humans as well as the rigid vertebral columns of apes. It is hypothesized that osteoarthritis is specific to humans due to our highly bendable spines. It is moreover further hypothesized that owing to their lack of functional mobility, the apes will not exhibit the extent of OA seen in the humans. MATERIALS AND METHODSSampleEach specimen examined was from the Hamann-Todd Osteological Collection at the Cleveland Museum of Natural History. The human sample consisted of 90 specimens spanning over 6 decades. The breakdown by age category was specimens ranging from ten 20 yearolds, twenty 30 year-olds, twelve 40 year-olds, twenty 50 year-olds, fifteen 60 year-olds, and ten 80 year-olds. Gender and race were noted as well. Forty-one females were examined (23 black, 18 white) and forty-six males (21 black, and 25 white). One Australopithecus (Lucy) was examined. From the African ape collection twelve gorillas (Gorilla) (6 male, 6 female) and twelve chimpanzees (Pan) (6 male, 6 female) were examined. In addition four orangutans (Pongo) (2 males, 2 females), two baboons (Papio) and four gibbons (Hylobates) were studied. Figure 1. this is a superior view of a L4 element showing prolific osteophyte formation on the vertebral body.
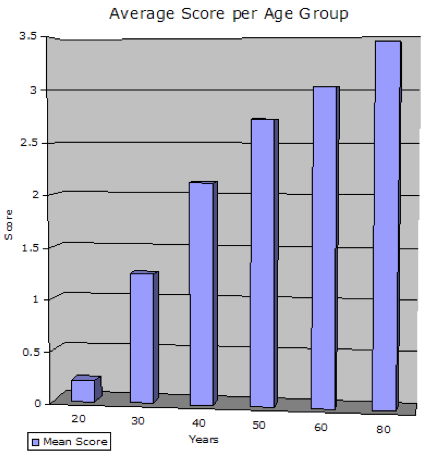
MethodEach specimen‟s thoracic and lumbar vertebrae were examined for the presence of OA. OA is characterized by the presence of osteophytes. Using a diagram which illustrated a lateral, superior and inferior view of the thoracic and lumbar vertebrae, arthritic development was noted on the facet joints, or the superior and inferior vertebral bodies. Any appearance of "lipping," or osteophyte formation (see Fig- 1), was noted on the corresponding diagram. Location, shape, size, and severity were recorded. The presence of Schmorl‟s nodes (a herniation through the intervertebral disc through the end-plate) (Schmorl 1930), infection, and previously scanned CT bone mineral densities were recorded as well. After each vertebra was closely examined and all manifestations of OA recorded, the degree of arthritis was then scored on a severity scale from 0-4. Zero indicated no osteophyte formation; one indicated very slight osteophyte formation; two indicated clear osteophyte formation; three indicated prominent osteophytes; and finally, four designates very extensive osteophyte formation, frequently resulting in the fusion of two or more vertebrae. Figure 2 illustrates the relationship between age and severity of osteoarthritis in humans. It is apparent that the severity of OA increases with age.
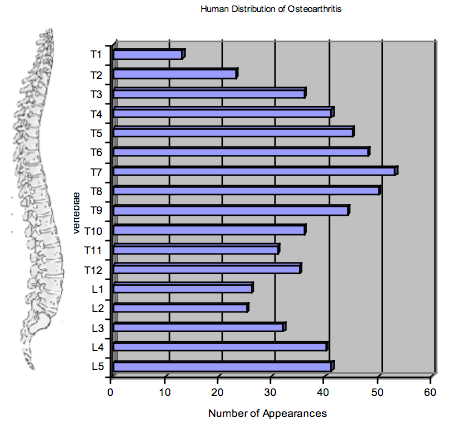
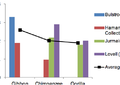
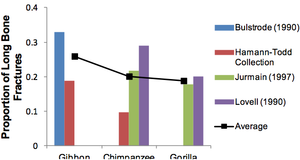
RESULTSAge vs. Severity of OA in HumansThe specimens examined were broken into age categories 20, 30, 40, 50, 60, and 80. The severity and prevalence of OA gradually increased with each decade. The human specimens began exhibiting minimal signs of OA during the third decade of life, and it progressed gradually up through age 80 (Fig. 2). Of the ten 20 year-olds examined only two (20%) of the ten exhibited any arthritis, both of which scored a 1. This yielded a mean score of 0.2. An increase in ten years results in a definite increase in the amount of arthritis. Of the twenty 30 year-olds that were examined, sixteen (80%) of the twenty exhibited at least some form of arthritis. When compared to the previous group (20year olds) a 60% jump in frequency of OA was noted. Of the twenty 30 year-olds, eight scored a 0, eight (40%) scored a 1, seven (35%) scored a 2, and the remaining specimen (5%) scored a 3. This yielded a mean score of 1.25. Of the 40 year-olds, eleven (91.6%) of the twelve specimens exhibited some form of OA. Only one specimen (8.3%) exhibited no arthritis, three (25%) scored a 1, three (25%) scored a 2, five (42%) scored a 3, and one (8.3%) scored a 3.5. This totaled a mean score of 2.13. Again, the arthritis continues to increase in severity from pro- gressive age group to age group. By the 6th decade of life, all twenty (100%) of the specimens exhibited some form of arthritis. The severity score also rose with a majority of thirteen (65%) out of twenty scoring a 3 or higher. The 50 year -olds had an average severity score of 2.73. Each 60 year-old specimen had arthritis and the mean score climbed to 3.03. Finally, the last age group, the 80 year-olds, as expected, exhibited the most extensive forms of OA. Six (60%) of the 80 year-old specimens displayed the most severe forms of OA, scoring the highest rating, 4. These rates yielded a final mean score of 3.45. These results indicate that OA is age-related, showing a definite increase in frequency and severity with time. (See Fig-2) OA in HumansFigure 3 displays the distribution of OA among the thoracic and lumbar vertebral elements. The prevalence of arthritis peaked at T7 which is anatomically located at the depth of the thoracic kyphosis. At T7 arthritis appeared a total of fifty-three (63%) out of eighty-nine times. After T7 the arthritis gradually decreases. However, there is a slight increase in prevalence at L4 and L5. Figure 3 illustrates the distribution of OA among the thoracic and lumbar elements. It is apparent that at T7 the frequency of OA is more prevalent.
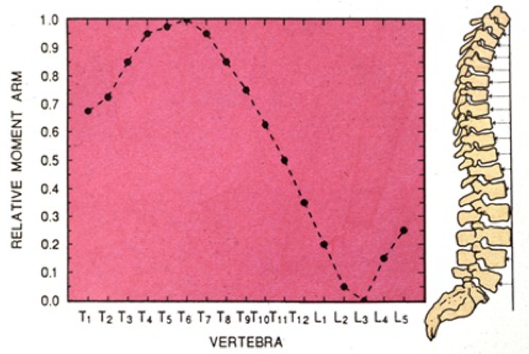
Figure 4 shows the distribution of relative moment arms among the various thoracic and lumbar vertebrae while under compression. The reason for the distribution seen in Fig-4 can be explained by looking at the human thoracolumbar column in lateral view. The vertebra subject to the greatest loads was T7. All other elements T1-L5 were measured with a moment arm relative to T7. Under compressive loading the mid thoracic spine bears the greatest bending stress. Interestingly, Figure4‟s graph of the thoracic and lumbar elements essentially mimics that of the OA distribution graph seen in Figure 3. They both peak at T7 and then drop off. However, there is a slight increase at L4 and L5 due to the lumbar lordosis. Figure 4 shows the moment arm‟s measurements of each vertebra under compression in relation to the T7th element. The moment arm is perpendicular to the bodyweight vector. Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |