The Rise of Global Health: How Did Health Become a Matter of Global Concern?
By
2016, Vol. 8 No. 06 | pg. 1/2 | » Despite being often overlooked within the discipline of International Relations (Lee, 2004: 29; Bambra et al., 2005: 187), the governance of health has become central to international politics. As recent spatial, temporal and cognitive transformations have developed from accelerated globalization, the determinants of health have become increasingly global and thus beyond the control of any individual nation-state.
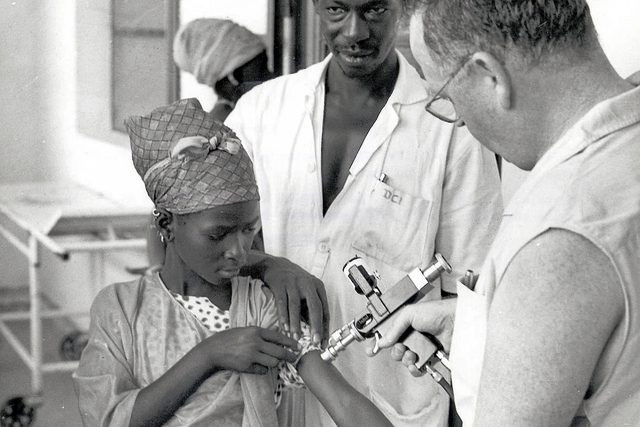
Historical image of a doctor administering the smallpox vaccine. Photo: WHO ND-2.
The aim of this essay is to examine developments within global health governance in order to illuminate the structural and political dynamics of how health has become a matter of global concern. I argue that although the transformation of global health governance has partially been driven by the structural imperatives of globalization, the highly unequal attention and resources devoted to certain health issues suggest such systemic forces are not alone in shaping the global health agenda. An account of the processes of political contestation between a wide variety of state and non-state actors is needed to explain differential responses to global health issues as well as the persistence of unequal health outcomes, reflecting the inherently political nature of global health governance. Understanding how both structures and actors influence global health can also illuminate the dynamics of global governance more generally, allowing for the identification of new strategies for international political contestation and collaboration. Recognizing the political nature of the globalization of health, rather than viewing it as an unstoppable natural force, paves the way for positive and equitable change in global health outcomes. Global health governance is often traced back to the mid-nineteenth century, when European states participated in the International Sanitary Conference of 1851 in order to standardize quarantine regulations, constituting one of the earliest multilateral responses to an international health issue (McKee et al., 2001: 7). Technological innovations and the confirmation of germ theory contributed to increased international cooperation in the late nineteenth and early twentieth centuries in order to prevent the spread of disease across national borders, leading to the creation of the International Sanitary Regulations in 1903 and the Office International d’Hygiène Publique in 1907 (Harman, 2014: 657). Such initiatives paved the way for broad interstate cooperation to tackle international health issues via the League of Nations Health Organisation in the inter-war period, and eventually the creation of an agglomeration of United Nations organisations, including the World Health Organisation (WHO) as ‘the global health institution’ in 1948 (Ibid.: 658, original emphasis), to promote better health outcomes globally after the Second World War. Global health governance, then, is by no means a recent development. However, the late twentieth and early twenty-first centuries have seen a significant increase in the rate and scope of changes brought about by globalization, affecting the nature of health determinants and outcomes, and consequently transforming the global health agenda. The acceleration of globalization towards the end of the twentieth century is evident in spatial, temporal and cognitive transformations, all of which affect health outcomes globally, and thus present challenges to the effective governance of health within and across states (Lee, 2004: 21). Innovations in transport and communications technologies, together with the post-1970s neoliberal world order marked by the promotion of free trade policies, have led to a spatial and temporal shrinking of the world, in which it has become difficult for individual states to control increasingly immense, complex and rapid trans-border flows of goods and people (Lee, 2001: 15-17). Such flows affect health both directly, by furthering the spread of pathogens across borders along with the movement of goods and individuals, and indirectly, as international trade contributes to economic development across the world, with obvious impacts on the capacity of states to ensure access to health care and address broader determinants of health such as poverty and education levels (Frenk et al., 2001: 31). Developed countries have experienced much more significant improvements in health outcomes than developing countries, and health gaps between high- and low-income population segments within countries persist. The cognitive dimension of globalization is reflected in the sharing of ideas and knowledge, thus deeply affecting how health issues are conceptualized and approached globally (Lee, 2001: 21). The challenges posed by globalization to health have been evident in the global scope and rapid spread of food, energy and economic crises in the twenty-first century, and the ways in which such crises have adversely affected health outcomes in various countries (Fidler, 2009). This is not to say that the effects of globalization on the governance of health have been entirely negative, as the transformations of the past few decades have also paved the way for positive developments in terms of knowledge and technology sharing, data gathering, and coordinated responses to global health crises (Garner & McKee, 2001: 202). Indeed, both the challenges and opportunities presented by the systemic forces of globalization must be taken into account in order to understand the dynamics of global health governance today. However, focusing solely on these structural imperatives can obscure the very unequal nature of the globalization of health, an understanding of which is crucial in order to explain why certain issues become privileged over others on the global health agenda. Although health outcomes have improved quite significantly on a global scale in terms of life expectancy, child death rates and nutrition levels, as well as access to water, sanitation and antenatal care, the distribution of these positive developments has, in fact, been deeply unequal (WHO, 2008: 6-7). Developed countries have experienced much more significant improvements in health outcomes than developing countries, and health gaps between high- and low-income population segments within countries persist (Bambra et al., 2005: 188). Moreover, vast amounts of resources are mobilized to tackle infectious diseases deemed threatening to developed countries, such as HIV and Influenza A H5N1 (avian flu), while diseases which contribute to many more deaths globally (e.g. diarrhoeal diseases), but the adverse effects of which are largely confined to developing countries, are neglected (Lee, 2004: 15-17; WHO, 2015). Indeed, only 10% of medical research and development expenditure seeks to address health issues that affect the poorest 90% of the global population (Elbe, 2007: 122). Such differences are the product of a global health governance regime that focuses on selective, rather than comprehensive, primary health care (Sanders & Chopra, 2003: 107). In other words, programmes of vertical, technocratic intervention in order to tackle specific health issues are privileged over horizontal approaches that aim to strengthen health systems more generally, and to address a wider range of the economic and political determinants of health, such as income, education, and employment conditions, among many other factors (Lee, 2004: 188-189). Furthermore, the globalization of health governance has been significantly shaped by the post-1970s neoliberal approach to health policies, which has sought to promote market forces as the determinants of health care provision and access, thus inevitably privileging the affluent over the poor (Harman, 2012: 5-6). The result of these influences has been a global health governance regime heavily skewed towards market-oriented, vertical approaches to health, in which economic and political power largely shape the global health agenda, and determine who has access to health care and who does not. Therefore, in addition to an account of the structural imperatives of globalization, we must look to the dynamics of political power and contestation involved in global health governance in order to explain differential health outcomes within states and across the globe. Intergovernmental organisations (IGOs) such as the WHO, the myriad UN organisations, and the World Bank, have played a central role in promoting interstate cooperation and coordination in order to tackle global health issues (Harman, 2012: 27). Such organisations can have an immensely valuable positive impact on health outcomes globally, as in addition to the direct provision of health services, research and aid, IGOs allow states to centralize information and data collection, take coordinated action in response to health issues, standardize procedures and provide frameworks for drafting international law (Harman, 2012: 35-37). Despite rhetoric of health as a global public good and a supposed focus on an equitable approach to health systems strengthening, however, these organisations have been marked by political contestation both within and between them (Davies, 2009: 28). Their relative influence in shaping the global health agenda, and the discourse used therein, is determined by relationships of political and economic power. Composed of member states and largely reliant on state funding, these organisations are often constrained by the national interests of their members. These inequalities have resulted in a focus on health issues deemed threatening to developed countries, such as infectious diseases (McInnes & Lee, 2006: 5), and a privileging of the economic interests of the industrialized world over the health interests of developing countries, evident in policies by the World Bank and World Trade Organisation (WTO), for instance, that work to reduce trade barriers in the developing world, despite often having adverse effects on local health outcomes and the strength of public health systems globally (Parker, 2002; Koivusalo, 2003). State-led organisations and initiatives, as well as interstate economic and political relationships, thus constitute central factors shaping the global health agenda. However, as the structural forces of globalization have created new political spaces for contestation and collaboration by undermining the capabilities of states to address the increasingly global determinants of health, focusing solely on states and IGOs does not allow for a comprehensive understanding of the political dynamics of global health governance. A reconceptualization of global health governance in order to transcend a state-centric approach has become increasingly vital, as a variety of influential non-state actors have challenged ‘the global playing field in health, its norms, its rules, its practices and above all its power politics’ (Kickbusch, 2003: 198). NGOs, such as Médecins Sans Frontières, have played an increasingly important role in reshaping the global health agenda from the bottom up (Orbinski, 2007; Jareg & Kaseje, 1998); the Bill & Melinda Gates Foundation, a private philanthropic organisation, has become a ‘global health power in its own right’ with assets that far surpass the annual budget of the WHO (Fidler, 2009: 3; Davies, 2009: 52); and private, profit-seeking corporations, are increasingly influential in setting the global trade policy agenda via the WTO (Garner & McKee, 2001: 198; Muzaka, 2009: 294).Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |