Featured Article:Controlling and Preventing HIV in Southern Africa
By
2009, Vol. 1 No. 10 | pg. 1/2 | »
IN THIS ARTICLE
KEYWORDS
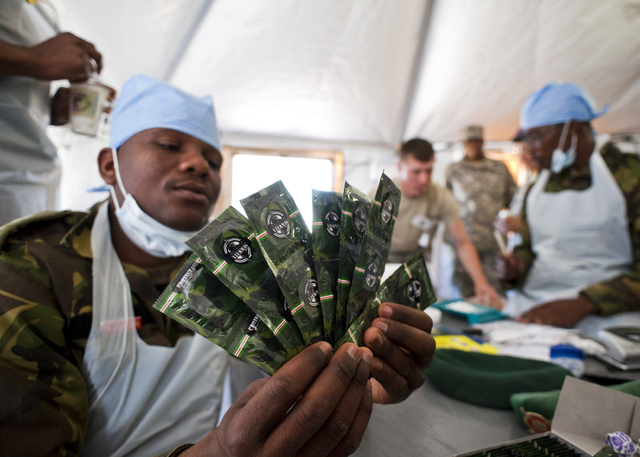
The Human Immunodeficiency Virus (HIV) originated in Africa. According to current estimates, the disease first infected humans in the 1930s, spreading outward in its formative years to the world beyond.6:1 It was nevertheless not until 1983 that the virus was first identified in France,13 by which time the virus was already well established in East and West Africa and mounting as the most significant challenge in Africa’s contemporary history. Since 1981, AIDS has caused 25 million deaths throughout the world.12:15 But the disease has been most acutely felt within the sub-region of Southern Africa, which claimed 67% of all HIV infections globally and 72% of the deaths in 2007. 12:5 The burden created by the AIDS epidemic in highly affected regions of Africa does not just represent a health problem. Rather, it has become a social, political, and economic challenge of the highest order. HIV/AIDS is inextricably linked in the chain of impoverishment and struggle that permeates many communities in sub-Saharan Africa.HIV/AIDS has become a social, political, and economic challenge of the highest order, linked inextricably in the chain of impoverishment and struggle that permeates many communities in sub-Saharan Africa. In recent years, the world has turned greater attention to this urgent problem. Numerous initiatives, originating in developed countries around the globe, have set out to stop the spread of HIV and reduce the suffering it inevitably causes. Sadly, and despite these myriad efforts, little progress has been made on a large scale. In some areas, new infection rates have stabilized at shockingly high levels; in other areas, new infections continue to grow. In only a few rare cases have HIV transmission rates in Africa been meaningfully reduced. Billions of dollars of funding and aid has been thrown, year after year, at a problem that seemingly will not respond. A Botswana Defense Force health specialist displays free contraceptives which are provided to local Monwane villagers in Botswana. The treatment and free contraceptives were provided to educate the public on safe sex practices and safe male circumcision. Photo: U.S. Army Africa. CC-2 Explaining HIV Rates in Southern AfricaIn order to identify the most effective methods of controlling the spread of HIV in Southern Africa, it is important to examine the various factors that have driven the unparalleled growth of the disease in the region. This region is unique in that it is the only area where HIV has reached and exceeded the status of a generalized epidemic in virtually all included countries.13:4-6 Other populations throughout the globe maintain the highest rates of HIV prevalence in concentrated sub-population groups deemed “high-risk” for contracting the virus. These groups include men who have sex with men (MSM), injection drug users (IDU), and sex-workers. These high-risk population groups are the only populations out of Africa that have historically reached HIV infection rates comparable with those in Southern Africa. For instance, in 1990 HIV prevalence for IDU reached 50% in Bangkok, Thailand while in the United States, “57 percent of AIDS cases were infected through male-to-male sex” in the 1990s.13:3-5 In both cases, HIV was generally restricted to high-risk population groups. However, in sub-Saharan Africa the disease has moved beyond high-risk populations. Many assertions have been made as to why HIV has spread rapidly in Africa, and although there are of course multiple dimensions to the problem, it is important to dispel the myths about HIV transmission. As Potts, et. al. write, “Devastating epidemics have frequently been attributed to poverty, limited health services, illiteracy, war, and gender inequity… but these grave problems… do not appear to be the immediate causes of generalized epidemics.”9:749 In this same vein, and contrary to conventional wisdom, recent studies actually found a direct relationship between wealth and HIV prevalence in Kenya. Other assumptions have been similarly unfounded, and overall fail to explain the variation in HIV prevalence that exists between Africa and other world regions. 9:749 In fact, available evidence suggests that the generalized epidemics in Southern Africa are the product of several critical variables, at the center of which is sexual behavior: “SADC and UNAIDS concluded that ‘high levels of multiple and concurrent sexual partnerships by men and women with insufficient consistent, correct condom use, combined with low levels of male circumcision are the key drivers of the epidemic in the sub-region.” 4:19 The prevalence of multiple concurrent partnerships appears to be a key driver of HIV in the region. Though Europeans and Americans tend to have comparable or even higher numbers of sexual partners in their lifetimes, these relationships are typically monogamous. As researchers found, even slight changes in this pattern can act to connect the sexual “web” that fuels the spread of HIV. Referring to a scientific model presented at Princeton University, one author writes: “A small increase in the average number of concurrent sexual partners -- from 1.68 to 1.86 -- had profound effects, connecting sexual networks into a single, massive tangle that, when plotted out, resembled the transportation system of a major city.”11 This trend leading to multiple partnerships has traditional roots. In many African societies it is highly respected for a man to take multiple wives, and significantly more common, when compared to other world regions, for both men and women to have ongoing, multiple, and concurrent sexual partnerships. For instance, in Lesotho, 55% of men “reported having two or more regular, ongoing (lasting at least a year) sexual partnerships in the previous year.”4:20 Women also reported higher than average rates of multiple concurrent partnerships. To underscore the importance of sexual behavior as a critical factor, one can look at the case of Uganda as an example. As of 1986, it was estimated that HIV prevalence in urban areas was as high as 29%.10 Urban regions were notorious for their sexual culture, in which it was commonplace for men and women to engage in casual sexual encounters on a recurring basis. However the Ugandan government, led by President Yoweri Museveni, took early action to encourage safe sexual behavior with the “Zero-Grazing” campaign in the late 1980s and early 1990s. At the core of the campaign was a message of behavior change, and the results were significant: “Men with three or more ‘non-regular’ partners in the previous year were reduced from 15% in 1989 to 3% in 1995.”35 This campaign led to a drop in adult HIV prevalence of greater than 50% over a roughly similar time period.4:22 Since the program was phased out in the mid 1990s, there has likewise been a relapse marked by an increase in the number of adults reporting multiple concurrent partners, and an increase in HIV prevalence.4:22 It is therefore clear that sexual behavior plays a central role in the fight against HIV. Another critical factor in the explanation of Southern Africa’s severe HIV rates is low levels of male circumcision (MC). The strong relationship between MC and HIV prevalence has been underemphasized in the past, but it nevertheless plays an important role: “Over 45 observational, biological, and other studies from the last 20 years have shown that MC significantly reduces risk of heterosexual HIV infection. The population-level effect of widespread MC is observed in west Africa, where HIV has been present for many decades, yet prevalence remains relatively low.” 9:750 The examination of various data sources shows that, throughout the region, in areas where MC is more common, HIV prevalence tends to be lower. 2 As an example, Potts, et. al. compared HIV rates and behavior in Niger, a Muslim country on the fringe of the AIDS belt; “sexual behavior is relatively restrained and MC is universal… Niger has an adult HIV prevalence of 0.7%, despite being the lowest ranking country in the Human Development Index.” 9:749 These two factors—sexual behavior and male circumcision—appear to play a key role in explaining differences in HIV prevalence between regions.Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |